Prevalence of Allergic Rhinitis by Age Group - PowerPoint PPT Presentation
1 / 29
Title:
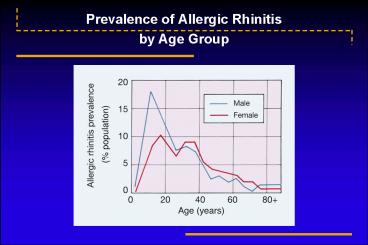
Prevalence of Allergic Rhinitis by Age Group
Description:
Atrophic (eg, cocaine abuse) Due to hormonal changes (eg, pregnancy) Nasal Obstruction ... Cells in Nasal Mucosa Mediators & Cytokines ... – PowerPoint PPT presentation
Number of Views:107
Avg rating:3.0/5.0
Title: Prevalence of Allergic Rhinitis by Age Group
1
Prevalence of Allergic Rhinitisby Age Group
2
Related Anatomic StructuresCompromised by
Allergic Rhinitis
3
Differential Diagnosis of Rhinitis and Nasal
Obstruction
- Rhinitis
- Allergic, seasonal, or perennial
- Infectious, chronic, or acute (frequent
recurrences) - Obstructive foreign body
- Secondary to topical decongestants (eg,
rhinitis medicamentosa) - Nonallergic with eosinophilia (NARES)
- Nonallergic vasomotor
- Atrophic (eg, cocaine abuse)
- Due to hormonal changes (eg, pregnancy)
- Nasal Obstruction
- Allergic or nonallergic rhinitis
- Rhinosinusitis
- Anatomic abnormality (eg, deviated septum)
- Nasal polyps
- Tumor (eg, angiofibroma)
- Cerebrospinal fluid leakage secondary to
perforation of the cribriform plate by
fracture or tumor - Granulomatous disorders (eg, Wegeners
granulomatosis, sarcoidosis) - Foreign body
4
Seasonal Allergic Rhinitis Mechanism of
Therapeutic Agents
- Cells in Nasal Mucosa Mediators Cytokines
- Antihistamines Decrease eosinophils Inhibit
histamine - and neutrophils release by blocking H1
- receptors
- Reduce expression of ICAM-1 Reduce PGD2 in nasal
- on epithelial cells secretions
- Nasal Decrease T cells (CD3, Decrease ECP,
- corticosteroids CD4, CD8), Langerhans
cells, histamine, tryptase, - mast cells, basophils, and IL-3, IL-5, and
GM-CSF - activated (EG2) eosinophils
- Attenuation in cell numbers after allergen
challenge - ECPeosinophil cationic protein
GM-CSFgranulocyte macrophage colony-stimulating
factor
5
First-generation Antihistamines
- H1 Sedative Anticholinergic GI
Blockade Effects Effects Effects - Ethylenediamines (tripelennamine)
- Ethanolamines (diphenhydramine)
- Alkylamines (chlorpheniramine)
- Piperazines (hydroxyzine)
- Piperidines (azatadine)
- Strongly positive effec
6
Second-generation Antihistamines
- H1 Sedative Anticholinergic GI
Blockade Effects Effects Effects - Fexofenadine (60 mg bid)
- Astemizole (10 mg qd)
- Loratadine (10 mg qd)
- Cetirizine (10 mg qd)
- Negative effect
- Strongly positive effect
7
Advantages of Second-generation Nonsedating
Antihistamines
- Bind strongly to histamine (H1) receptors
- negligible affinity for nonhistamine receptors
- no anticholinergic effects
- Do not cross the blood-brain barrier
- do not affect cognitive functions or
psychomotor performance - do not potentiate impairment caused by alcohol
or benzodiazepines - do not impair driving skills
8
Treatment of SAR With Fexofenadine Safety
(N575)
- No sedation
- No ECG abnormalities
- including no prolongation of QTc at 60, 120, or
240 mg bid - 60-mg bid dose optimal
- frequency of adverse events similar among all
groups
9
Safety and Efficacy of Once-a-day Dosage for
Adult SAR
10
Once-a-day Fexofenadine for Adult SARAdverse
Events (gt2)
- Fexofenadine HCI, N
() - Placebo 120 mg 180 mg Total Active N293 N287 N
283 N570 - EffectOverall occurrence 88 (30.0) 86 (30.0) 86
(30.4) 172 (30.2) - Headache 22 (7.5) 21 (7.3) 30 (10.6) 51 (8.9)
- Upper respiratory 9 (3.1) 6 (2.1) 9 (3.2) 15
(2.6)tract infection - Pharyngitis 9 (3.1) 8 (2.8) 6 (2.1) 14 (2.5)
- Back pain 4 (1.4) 8 (2.8) 8 (2.8) 16 (2.8)
- Pain 10 (3.4) 7 (2.4) 5 (1.8) 12 (2.1)
11
Decongestants
- Actions
- Constrict mucous membranes shrinkage promotes
drainage, improves ventilation, relieves
nasal stuffiness - Routes of administration
- Systemic, topical
- Indications
- Allergic rhinitis, vasomotor rhinitis, sinusitis,
eustachian tube congestion - Side effects
- Systemic stimulation (CNS, cardiovascular)
- Topical rhinitis medicamentosa, CNS stimulation,
local irritation
12
Drugs for Pediatric Allergy (lt12 years)
- Antihistamines
- Brompheniramine maleate
- Cetirizine
- Chlorpheniramine maleate
- Clemastine fumarate (12-hour liquid)
- Diphenhydramine HCl
- Loratadine
- Decongestants
- Phenylephrine HCl
- Phenylpropanolamine
- Pseudoephedrine
- Antihistamine/decongestants
- Chlorpheniramine maleate/
phenylpropanolamine - Brompheniramine maleate/ pseudoephedrine
- Intranasal preparations
- Nonsteroid Cromolyn sodium
- Corticosteroid Beclomethasone (AQ and
aerosol) Budesonide (aerosol) Flunisolide
(AQ) Fluticasone (AQ)
13
Safety of a Second-generation Antihistamine in
Children
Most Frequently Reported (?2) Adverse Even
Fexofenadine HCl (bid)
Placebo N () N () 15 mg 30 mg 60
mg Total (N229) (N224) (N209) (N213) (N646)
Total occurrence 83 (36.2) 79 (35.3) 77 (36.8) 73
(34.7) 230 (35.6) Headache 15 (6.6) 18 (8.0) 15
(7.2) 20 (9.4) 53 (8.2) URTI 4 (1.7) 11 (4.9) 9
(4.3) 3 (1.4) 23 (3.6) Pharyngitis 9 (3.9) 9
(4.0) 6 (2.9) 6 (2.8) 21 (3.3) Coughing 3 (1.3) 3
(1.3) 8 (3.8) 5 (2.3) 16 (2.5) Injury, accident 3
(1.3) 4 (1.8) 6 (2.9) 9 (4.2) 19 (2.9) Abdominal
pain 8 (3.5) 6 (2.7) 4 (1.9) 5 (2.3) 15
(2.3) Fever 2 (0.9) 4 (1.8) 5 (2.4) 4 (1.9) 13
(2.0)
URTI upper respiratory tract infection
14
Safety of a Second-generation Antihistamine in
Children
Frequency of ECG Outliers
-
Fexofenadine HCl (bid) - Placebo N ()
- N () 15 mg 30 mg 60 mg
- ECG Parameter (N229) (N224) (N209) (N213)
- PR (gt200 msec and 0 0 0 1 increase gt20 msec)
- QTc (gt450 msec and 7 6 6 3 increase gt10 msec)
15
Symptoms of Chronic Sinusitis in Children
- Symptom Occurrence ()
- Chronic nasal obstruction 100
- Purulent nasal discharge 90
- Headache 90
- Cough 71
- Fetid breath 67
- Postnasal drainage 63
- Behavioral changes 63
16
Sinus Areas Susceptible to Infection
17
Allergy vs Infectious Sinusitis Symptoms in
Children
- Allergy
- Itching of eyes, nose, and palate
- Clear rhinorrhea
- Sneezing
- Other symptoms
- eczema
- food allergy
- Infection
- Purulent anterior rhinorrhea or postnasal drip
- Frequent head pain
- Other
- intractable cough
- sore throat
- purulent sputum
18
Treatment of Pediatric Chronic Sinusitis
- Decongestants
- Antihistamines
- Antibiotics
- Amoxicillin (40 mg/kg tid 14-21 days)
- Amoxicillin-clavulanate (40 mg/kg tid)
- Azithromycin (10 mg/kg day 1 5 mg/kg days 2
to 5) - Cefixime (8 mg/kg qd or bid)
- Cefuroxime axetil (20-30 mg/kg bid)
- Clarithromycin (15 mg/kg bid)
- Loracarbef (30 mg/kg bid)
- Trimethoprim/sulfamethoxazole (8 mg/kg TMP and 40
mg/kg SMX bid) - Functional endoscopic sinus surgery
- Immunotherapy
19
Pathogenesis of Otitis Media With Effusion
20
Pathogenesis of Otitis Media With Effusion
(contd)
21
Risk Factors Associated With Otitis Media
- Viral URT infection
- Allergic rhinitis
- Eustachian tube dysfunction
- Cigarette smoking by parents (especially
mother) - Bottle feeding (questionable)
- Male gender
- Immunologic deficiency
- Ciliary dysfunction
- Adenoidal hypertrophy
- Cleft palate disorders
- Genetic predisposition
22
Tympanic Membrane Changes and Symptoms
- A. Normal
B. Affected by OME
23
Treatment of Otitis Media
- Antibiotics
- First choice amoxicillin
- Amoxicillin/clavulanate
- Erythromycin/sulfisoxazole
- Cephalosporin (for ?-lactamase- producing H
influenzae or M catarrhalis) - Clarithromycin or azithromycin (for suspected
penicillin-resistant S pneumoniae) - Decongestants
- For coexisting allergic rhinitis
- Antihistamine/decongestants
- Intranasal corticosteroids
- Intranasal cromolyn
- Allergen immunotherapy
- Follow-up physical examination
- Other measures
- Tympanometry (persistent OME)
- Antibiotic prophylaxis
24
Asthma and Allergic Rhinitis
25
Environmental Allergens and Childhood Asthma
- Dust mites
- Furry pets
- Molds
- Cockroaches
26
Compliance With Environmental Control Measures
- Response
- Dust my house frequently 34.1
- Do not have pets inside my house 20.8
- Avoid outdoor activities 18.7
- Wash bedding in hot water 15.0
- Wrap mattresses in plastic cover 6.0
- Do not have carpeting (or rugs) in my house 2.1
- No measures 25.4
- Note Respondents (481 patients with
self-reported allergic rhinitis) were asked to
check all items that apply.
27
Drug Compliance Rates Allergy and Asthma
- Noncompliance rates significantly high
- estimated 50 to 80 noncompliance
- Factors in treatment success
- education/clear communication write it down
- simplicity of dosing schedule
- minimal adverse effects, especially
cognitive/behavioral
28
Noncompliance Among Pediatric Patients
- Poor physician communication with
parents/caregivers - Inconvenient or complex dosing schedules
- Troublesome adverse effects
- Cost not affordable
29
Strategies to Encourage Compliance in Pediatric
Patients
- Educate regarding allergen avoidance measures
- Promote the need for medication compliance
- Enlist parental support
- Seek allergy specialist care